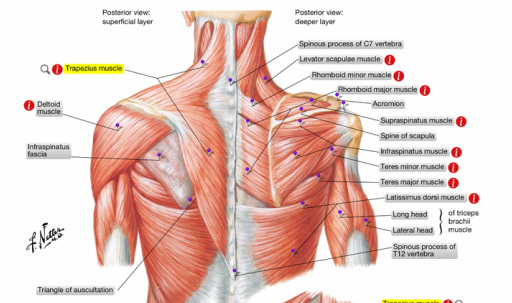
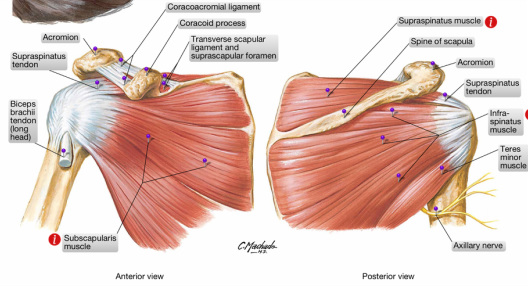
Radiology
Did you know?
1) The anatomic reason the aorta is relatively close to the umbilicus?
2) The clinical significance of a cervical rib?
5) The importance of popliteal artery aneurysms?
6) The location and clinical usefulness of the sural nerve?
7) The anatomic landmarks for lumbar puncture ( spinal tap or to administer a spinal anesthetic )?
8) What the piriformis syndrome is?
9) The clinical significance of the small saphenous vein?
10) How to visually diagnose a hip fracture?
1) The anatomic reason the aorta is relatively close to the umbilicus?
- The normal lumbar lordosis positions the aorta relatively close to the umbilicus making it vulnerable to laparoscopic port insertion injury.
2) The clinical significance of a cervical rib?
- Cervical ribs not uncommonly arise off of C7 and can cause thoracic outlet syndrome by narrowing the exit of the subclavian artery, vein or brachial plexus. They can be visualized on a plain chest X-ray.
- It is a network of valveless veins that connect the deep pelvic and thoracic veins to the internal vertebral plexuses. This provides a route for hematogenous spread of breast, bladder and prostate cancers to the vertebral column or brain. Named after Oscar Batson of Penn Anatomy Dept. who first described it in 1940.
- Occlusion by atherosclerosis or surgical trauma can cause spinal cord ischemia with paraplegia and loss of bladder and rectal control. It arises from a left posterior intercostal artery and supplies the lumbar and sacral cord. Can be occluded during repair of thoraco-abdominal aortic aneurysms.
5) The importance of popliteal artery aneurysms?
- They rarely rupture but often embolize clot distally, threatening the viability of the lower leg and foot. They are often bilateral and associated with abdominal aortic aneurysms. Can also cause tibial nerve pressure and popliteal vein pressure causing pain, edema and DVT ( deep vein thrombosis ). Treatment is surgical ligation & bypass or endovascular stenting if > 2 cm.
6) The location and clinical usefulness of the sural nerve?
- The sural nerve is formed by the junction of the medial sural cutaneous with the fibular anastomotic branch of the lateral sural cutaneous nerve. It lies close to the lesser saphenous vein and runs down to the interval between the lateral malleolus and calcaneus. It is cutaneous and its removal results in a relatively trivial deficit. It is often used for nerve biopsy to diagnose several diseases as well as a donor nerve for nerve grafting.
7) The anatomic landmarks for lumbar puncture ( spinal tap or to administer a spinal anesthetic )?
- With the patient in the lateral decubitus position ( i.e., lying on their right or left side ) with the back flexed, extend & adduct all your fingers. Place tip of 5th finger on top of iliac crest and your thumb will be at approximately L3 or L4. Since cord in adults ends at L2, this is a safe place for needle entry through the dura.
8) What the piriformis syndrome is?
- Muscle shortening or spasm of the piriformis can compress the sciatic nerve beneath it. In 17% of population, the common fibular nerve actually passes through the muscle. Gluteal weakness can also cause piriformis to hypertrophy. Can also be due to overuse in rowing or cycling. Suspect when sciatica occurs without spine pathology. Treatment is NSAIDS, stretching and physical therapy.
9) The clinical significance of the small saphenous vein?
- Valvular incompetence here can be a cause of posterior calf varicosities and it can also be harvested for arterial bypass purposes if great saphenous unavailable or phlebitic.
10) How to visually diagnose a hip fracture?
- The lower limb will be externally rotated due to unopposed action of the external rotators and limb is also shortened due to muscle spasm. Can suspect diagnosis simply by looking at a supine patient’s feet.
R2 & L2
|